Sinus Pain vs. Tooth Pain — How We Tell the Difference
Patient Profile
Torrance patient with discomfort in the upper right area after chewing, coinciding with active sinus issues
Clinical Challenge
Differentiating between sinus-related referred pain and a subtle underlying endodontic problem in a complex diagnostic presentation
Approach
Detailed patient history discussion and CBCT imaging for precise evaluation of multiple teeth and surrounding structures
Outcome
Identified potential endodontic issue; patient informed and reassured with a clear monitoring plan
The Case
The patient presented with two weeks of discomfort in the upper right area after chewing, coinciding with nasal congestion and sinus pressure during the holiday season. The referring question was straightforward but the answer wasn't: was this a dental problem, a sinus problem, or both?
This overlap is common. Upper posterior roots sit near or within the sinus floor, so sinus infections can mimic pulpitis and dental infections can cause sinus symptoms. Without targeted investigation, the source is often impossible to isolate.
What We Did
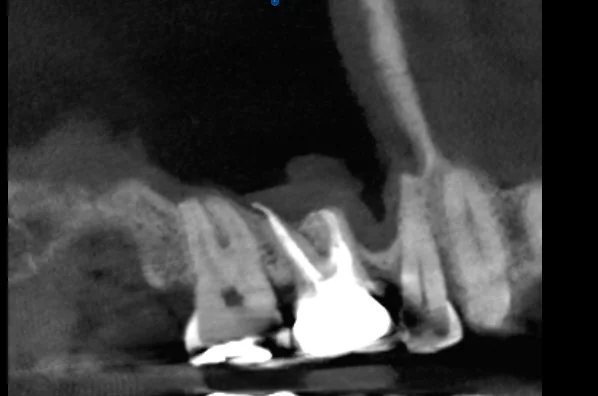
Our 30-minute consultation followed a systematic approach: detailed history taking (symptom timeline, aggravating factors, relationship to sinus congestion), clinical testing of all teeth in the affected quadrant (vitality, percussion, palpation), and CBCT imaging to evaluate teeth and sinus simultaneously in three dimensions—something standard radiographs cannot do.
What We Found
The CBCT scan revealed subtle signs of a potential endodontic concern in one tooth that was invisible on standard radiographs. The sinus appeared mildly thickened but without frank infection. The critical distinction: two overlapping conditions—one dental, one sinus—each requiring a different management approach.
The Plan
Rather than treat immediately, we chose a conservative path: monitor the tooth with follow-up testing in 3 months, coordinate with the patient's physician for the sinus issues, and return immediately if symptoms change. This preserved the option to intervene only if the endodontic concern progressed—avoiding an unnecessary root canal if the sinus was driving the symptoms.
Why This Approach Mattered
If we had rushed to treat, the likely outcome would have been a root canal that didn't resolve the patient's symptoms, because the sinus issue—not the tooth—may have been the primary pain driver. The patient would have undergone an invasive procedure, the actual sinus problem would have continued untreated, and resolving the sinus first might have eliminated the dental symptoms entirely.
Watchful waiting with a clear follow-up plan is sometimes the most responsible clinical decision.
Why CBCT Was Decisive
CBCT imaging allowed us to:
- Evaluate both teeth and sinus in a single scan
- Detect early pathological changes invisible on periapical radiographs
- Map root proximity to the sinus floor precisely
- Establish a three-dimensional baseline for monitoring changes over time
Key Takeaways
Clinical Insights
- Comprehensive consultations resolve diagnostic uncertainty: A 30-minute specialist consultation with appropriate imaging can prevent months of misguided treatment when symptoms overlap between dental and non-dental causes.
- CBCT imaging sees what 2D radiographs miss: For ambiguous upper posterior presentations, three-dimensional imaging should be standard of care.
- Watchful waiting is a valid treatment plan: Early or ambiguous pathology should be monitored with clear follow-up protocols rather than treated prematurely.
When to Refer for Specialist Consultation
General dentists should consider endodontic consultation when:
- Pain presentation doesn't match the expected pattern for a specific tooth
- Multiple teeth in the same area test borderline on vitality testing
- Upper posterior symptoms coincide with sinus congestion
- Standard radiographs are inconclusive and CBCT is needed for diagnosis
- The patient has had previous treatment in the area that complicates assessment
- You're not confident in the diagnosis—uncertainty is a valid reason to refer
Bottom Line: A comprehensive specialist consultation doesn't always result in treatment—and that's the point. The value lies in diagnostic clarity: knowing exactly what's happening, what needs treatment, and what can be safely monitored. For this patient, 30 minutes of specialist time prevented unnecessary dental work and provided the reassurance that comes from a definitive diagnosis.
Clinical Disclaimer: These cases are presented for educational purposes and published with appropriate patient consent. Patient identifying information has been removed in compliance with HIPAA regulations. Individual results may vary. All radiographic images and case descriptions represent actual patient treatment outcomes.
Procedures We Use for These Cases
The expertise demonstrated in these cases comes from mastering advanced endodontic procedures
Related Articles
Learn more about these treatments from Dr. Phan
 Cracked Teeth
Cracked Teeth Cracked Tooth: Crown, Root Canal, or Extraction? How We Decide
Not all cracked teeth need the same treatment. Dr. Jason Phan explains the 5 types of cracks, which ones can be saved, and how a microscope and CBCT determine the right treatment.
 Surgery & Retreatment
Surgery & Retreatment Failed Root Canal: Should You Try Retreatment or Get an Implant?
Your root canal didn't work — now what? Dr. Jason Phan compares retreatment vs. extraction and implant: success rates, costs, timelines, and how to decide which is right for your tooth.
 Root Canal
Root Canal Root Canal vs. Implant: Which Is the Better Investment for Your Tooth?
Choosing between saving your tooth with a root canal or extracting and replacing it with an implant? Dr. Jason Phan compares cost, success rates, timelines, and long-term outcomes.
 Root Canal
Root Canal Persistent Pain After Root Canal: Causes, Evidence, and When Retreatment Is Needed
A detailed clinical guide to understanding why pain persists after root canal treatment. Dr. Jason Phan covers odontogenic and nonodontogenic causes, diagnostic approaches, and evidence from current research.
 Consultation
Consultation What Happens During an Endodontic Consultation
Nervous about seeing an endodontist? Dr. Jason Phan walks you through exactly what happens during a consultation at our Torrance office — from the exam to the treatment plan.
 Pain Diagnosis
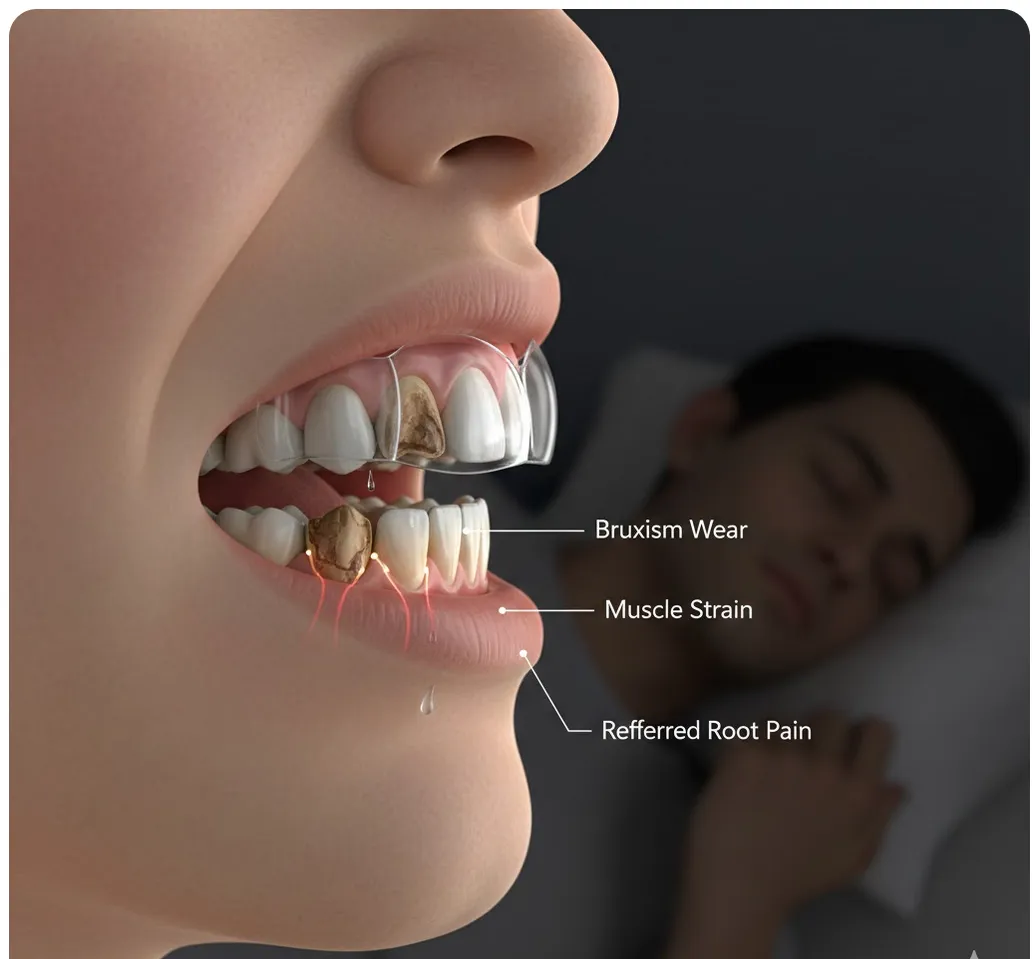
Pain Diagnosis Bruxism Pain Mimicking Root Canal Pain: When Grinding Feels Like a Toothache
Teeth grinding and clenching can cause tooth pain that mimics root canal symptoms. Dr. Jason Phan explains how a CBCT consultation in Torrance prevents unnecessary treatment.
 Pain Diagnosis
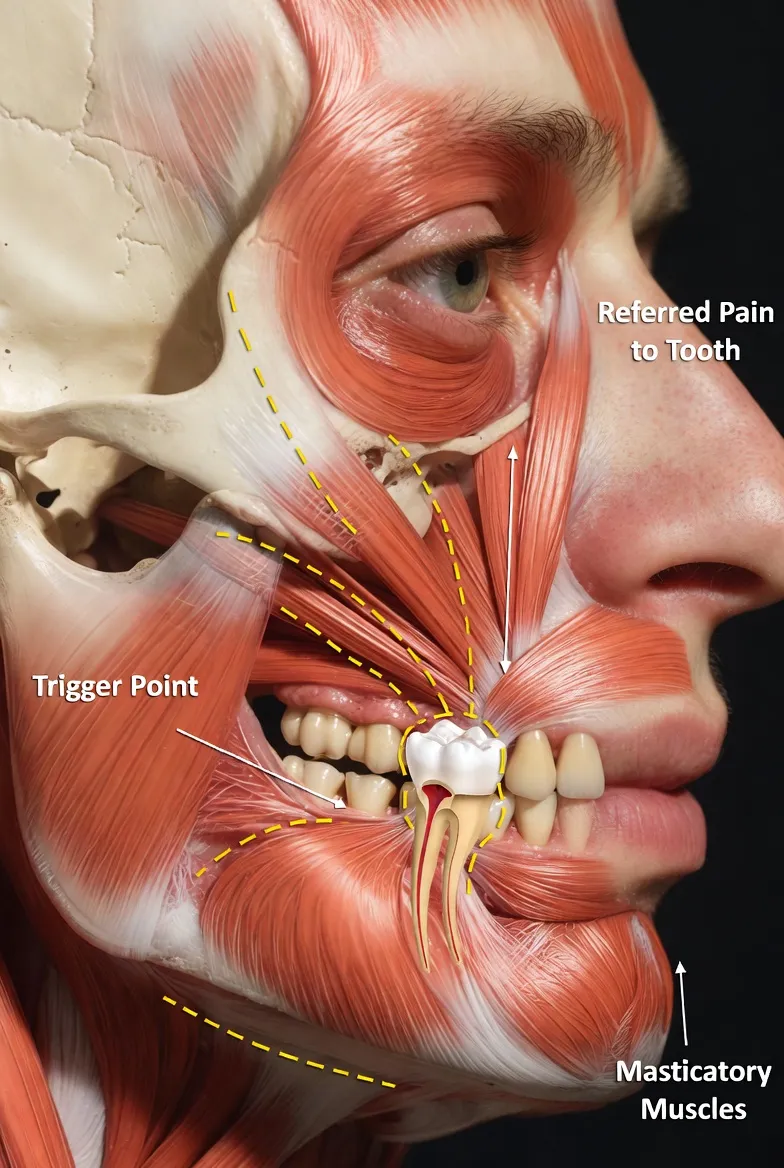
Pain Diagnosis Myofascial Pain Mimicking Root Canal Pain: When Jaw Muscles Cause Toothaches
Jaw muscle trigger points can refer pain to teeth, mimicking a root canal problem. Dr. Jason Phan explains how a detailed CBCT consultation in Torrance prevents misdiagnosis.
 Pain Diagnosis
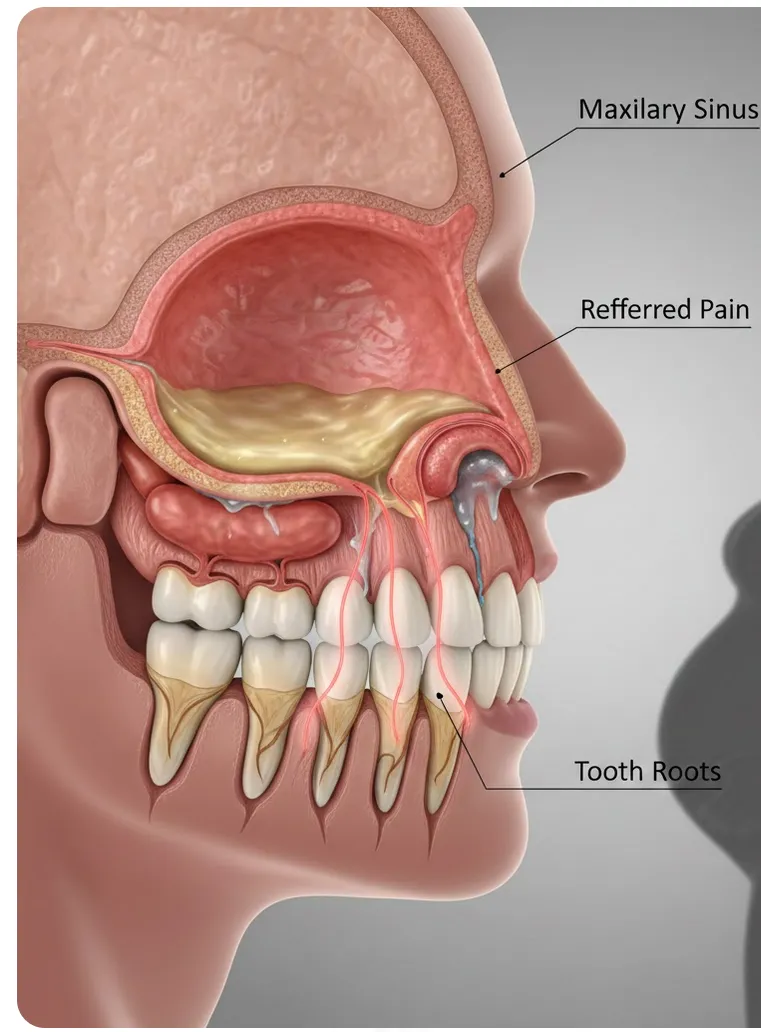
Pain Diagnosis Sinus Pain Mimicking Root Canal Pain: How to Tell the Difference
Maxillary sinusitis can cause tooth pain that feels like a root canal is needed. Dr. Jason Phan explains how CBCT imaging and thorough evaluation in Torrance prevent misdiagnosis.
 Pain Diagnosis
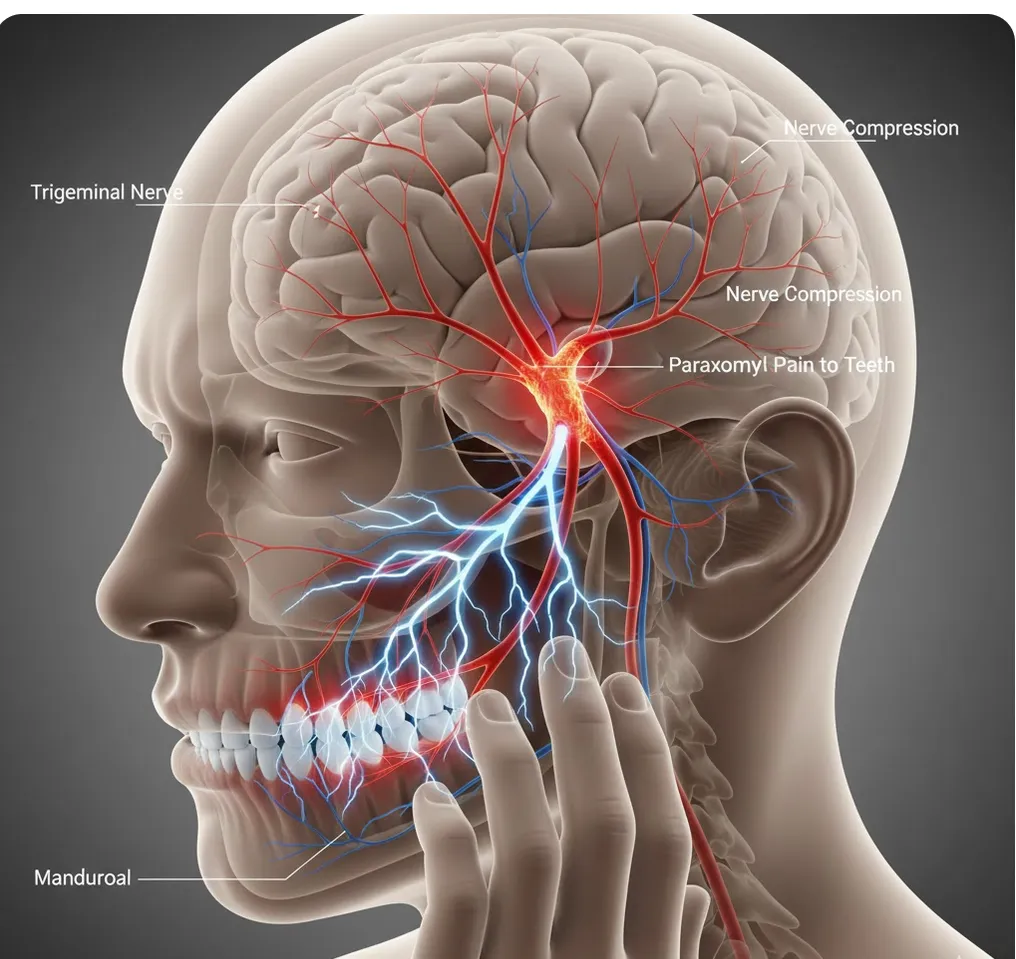
Pain Diagnosis Trigeminal Neuralgia & Other Nerve Conditions Mimicking Root Canal Pain
Trigeminal neuralgia causes intense facial pain often misdiagnosed as tooth problems. Dr. Jason Phan explains how CBCT consultation in Torrance prevents unnecessary root canals.
 Root Canal
Root Canal Endodontist vs. Dentist for Root Canal: 95% vs. 85% Success Rate
Endodontists have a 95–97% root canal success rate vs. 85–90% for general dentists. See the full comparison of training, equipment, cost, and when the specialist difference matters most.
 Pain Diagnosis
Pain Diagnosis Shingles Presenting as Tooth Pain: What You Need to Know
Shingles can mimic tooth pain, leading to unnecessary dental procedures. Dr. Jason Phan explains how herpes zoster affects the trigeminal nerve, the signs to watch for, and when to seek treatment.
Experience Matters in Complex Endodontics
When you refer patients to us, they benefit from decades of experience with the most challenging cases. We're here to help when routine endodontics isn't enough.
Mon-Fri: 8am-5pm | 23451 Madison St., Suite 210, Torrance, CA